Ear Infections in Kids (Acute Otitis)
Ear Infections in Children
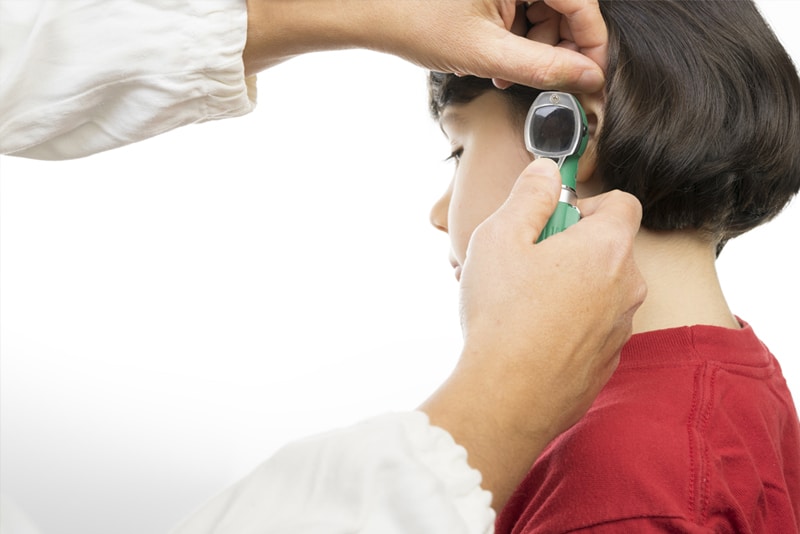
1. Acute Otitis Externa (Ear Canal Infection)
What are the Risk Factors for Acute Ear Infection?
- Cleaning the ear canal removes ear wax. Ear wax serves to protect the ears from water, bacteria, and injury. Excessive cleaning or scratching can injure the skin, potentially leading to infection.
- Swimming on a regular basis removes some of the ear wax, allowing water to soften the skin. Bacteria, which normally live in the ear canal, can then enter the skin more easily.
- Wearing devices that block the ear canals, such as hearing aids, headphones, or ear plugs, can increase the risk of acute ear canal infection (if worn frequently) by injuring the skin.
What are the Symptoms of Acute Ear Infection?
- Pain in the outer ear, especially when the ear is pulled or moved
- Itchiness of the ear
- Fluid or pus leaking from the ear
- Difficulty hearing clearly
How is Acute Ear Infection Diagnosed?
What is the Treatment for Acute Ear Infection?
- Lie your child on the side or ask him/her to tilt his/her head towards the opposite shoulder.
- Place the ear drops in the ear canal.
- Lie on the side for 20 minutes
How to Prevent Acute Ear Infection?
- Ask your child to shake his/her ears dry after swimming.
- Blow-dry your child’s ears on a low setting, holding the dryer 12 inches away.
- Consider wearing ear plugs made for swimming.
2. Acute Otitis Media (Middle Ear Infection)
What is a Middle Ear Infection?
What are the Symptoms of Middle Ear Infections?
- Fever
- Pulling on the ear
- Fussiness or irritability
- Decreased activity
- Lack of appetite or difficulty eating
- Vomiting or diarrhea
- Draining fluid from the outer ear (called otorrhea)
How is a Middle Ear Infection Diagnosed?
What is the Treatment for Middle Ear Infection?
- Antibiotics
- Medicines to treat pain and fever
- Observation
- A combination of the above
- If the child is older than 24 months
- If ear pain and fever are not severe
- If the child is otherwise healthy
What are the Potential Complications of a Middle Ear Infection?
One of the common complications of an ear infection is rupture (perforation) of the ear drum, also known as the tympanic membrane. The tympanic membrane can rupture when fluid presses on the membrane, reducing blood flow and causing the tissue to weaken. It does not hurt when the membrane ruptures, and many children actually feel better because pressure is released. Fortunately, the tympanic membrane usually heals quickly after rupturing, within hours to days. Rupture of the ear drum is an indication for antibiotic treatment of an ear infection.
The fluid that collects behind the eardrum (called an effusion) can persist for weeks to months after the pain of an ear infection resolves. An effusion causes troubled hearing, which is usually temporary. If the fluid persists, however, it may interfere with the process of learning to speak. Effusions usually resolve over time without any treatment. However, if the effusion persists for more than three months, the child may need treatment with a surgical procedure. The decision to treat is based upon how much the effusion affects the child’s hearing and the child’s risk of speech problems. Children with underlying speech, hearing, or developmental problems may have worse outcomes related to the fluid and conductive hearing loss. They may need earlier intervention. Children who are not treated for an effusion should be monitored over time. This includes an ear exam and hearing testing every three to six months until the effusion goes away.

